It’s well known that iron is a nutrient of concern in pregnancy. Iron is a mineral that is needed to make hemoglobin, a protein found in red blood cells that helps transport oxygen through your body. Too little iron can lead to low hemoglobin, which ultimately can cause anemia.
During pregnancy, you create more red blood cells to support yourself and your growing baby. Plus, those red blood cells turnover faster. This means that you need more iron — about 1.5 times more — to account for this increase in red blood cells.
Most care providers test for anemia during pregnancy and although iron deficiency is not the only cause of anemia, it’s one of the more common nutritional causes; other contributors include vitamin B12, folate, copper, and retinol. If they suspect you need more iron, you’ll likely be advised to increase your intake of iron-rich foods (or add a supplement).
But sometimes the recommended lists of iron-rich foods aren’t exactly the most bioavailable sources of iron.
Very early in my career, I took on a role as a prenatal dietitian and “inherited” the nutrition handouts from the dietitian I was replacing. The handout on iron prominently featured items like dark leafy greens, beans, and fortified cereals. But are these really the best ways to improve iron status?
What was missing from these handouts was any discussion on the total iron content of those foods relative to one another and also the bioavailability of iron, which can vary quite a bit! It never answered the question: How much iron do you actually absorb from food?
In this article, I’ll cover the different forms of iron and respective bioavailability, iron concentrations in different foods, and how much iron you actually absorb from food. Plus, we’ll cover some ways to enhance iron absorption from foods and how to improve your body’s ability to utilize iron (hint: complementary nutrients are key!).
Keep reading to learn more about iron and pregnancy.
Iron Needs in Pregnancy
In pregnancy, as your body builds new life, the amount of iron needed to support this function increases significantly.
Let’s look at the numbers. Women who are not pregnant need about 18 mg/day of iron. Compare this to women who are pregnant – they need about 27 mg/day. That’s quite a bit more!
Now, your body has some built-in systems to support iron status during pregnancy. Your body not only absorbs more iron from your food, but it also increases iron recycling within the body. Still, iron deficiency remains a common concern during pregnancy. Enhanced iron absorption and iron recycling are sometimes not enough to prevent deficiency.
Inadequate iron intake during pregnancy is a risk factor for numerous pregnancy complications, including preeclampsia, hypothyroidism, and preterm birth. It may also impair fetal brain development, stunt growth, and increase your baby’s lifetime risk of obesity, diabetes, and high blood pressure. This is why it’s crucial to improve iron status (if you can, prior to conception!!). If you’re already pregnant and are lacking in iron, now is definitely the time to improve your iron status!
The Challenge With Iron Supplements During Pregnancy
To prevent deficiency or improve iron status, it’s important to understand the different forms of iron you can consume.
As I mentioned earlier, you can absorb iron from the foods you eat, or you can take an iron supplement. Iron supplements may seem like the perfect hack, but there’s more to the story here. Sometimes iron supplements are not absorbed well, or they can cause unwanted gastrointestinal side effects (especially if you’re taking ferrous sulfate or ferrous fumarate forms). So even if you take a dose that seems adequate, you might not actually be absorbing all of the iron that you need.
The form known as iron bisglycinate is better absorbed, but not everyone needs an iron supplement in pregnancy. Plus, stand alone iron supplements don’t have all of the co-factor nutrients to help your body actually utilize the iron you’re taking in.
This is why I believe it’s important to focus first on iron intake from food before resorting to supplementation. But you also want to be aware of the different types of iron in foods, as this dramatically influences how much of that iron your body can actually absorb.
How Much Iron Do You Actually Absorb From Food?
Types of Iron in Foods: Heme Iron and Non-Heme Iron
There are two types of iron that are found in foods: heme iron and non-heme iron.
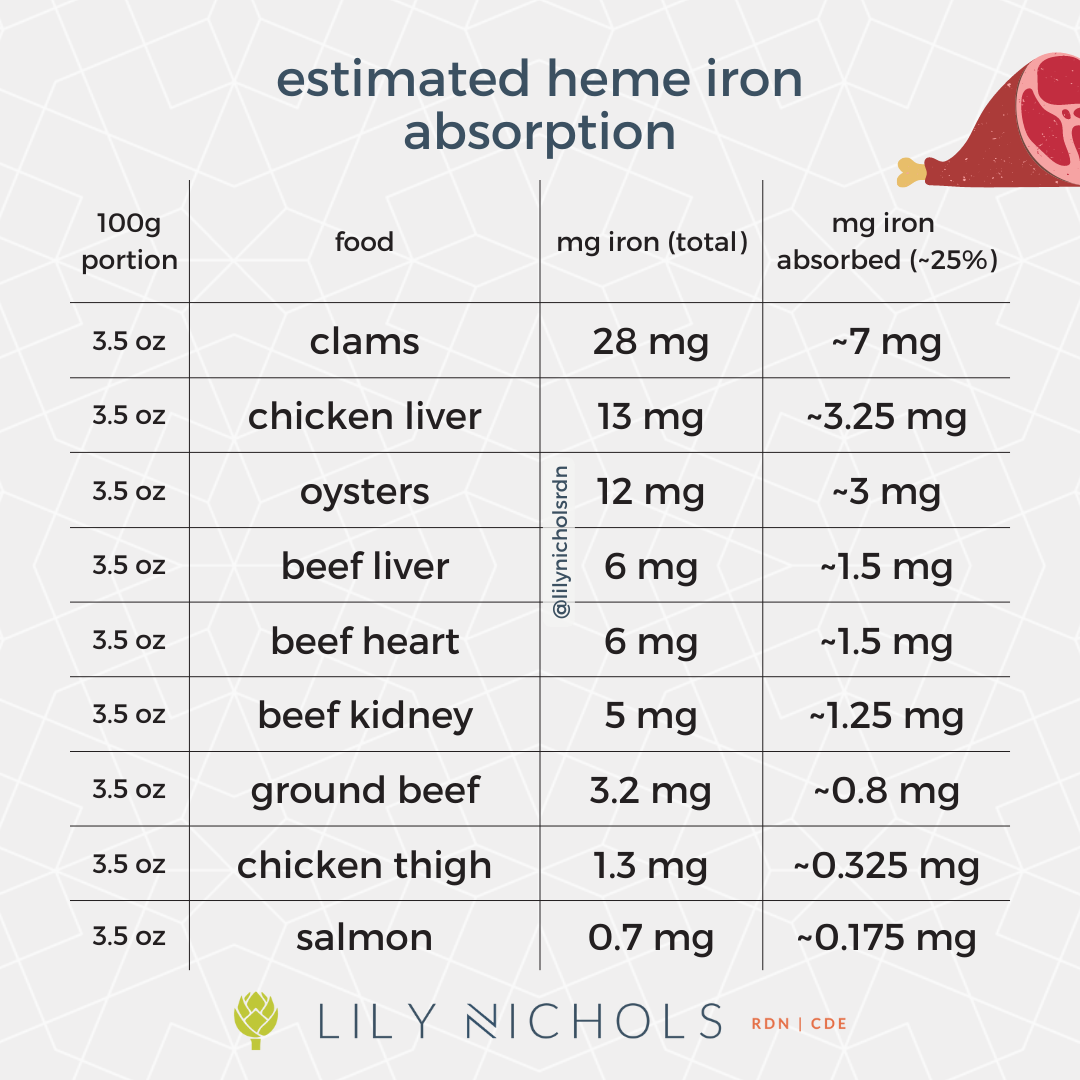
Heme iron is iron found only in animal foods, since heme is made in the bone marrow and liver. Some examples of foods rich in heme iron per 100 g serving are: clams, chicken liver, oysters, beef liver, beef heart, beef kidney, ground beef, chicken thigh, and salmon.
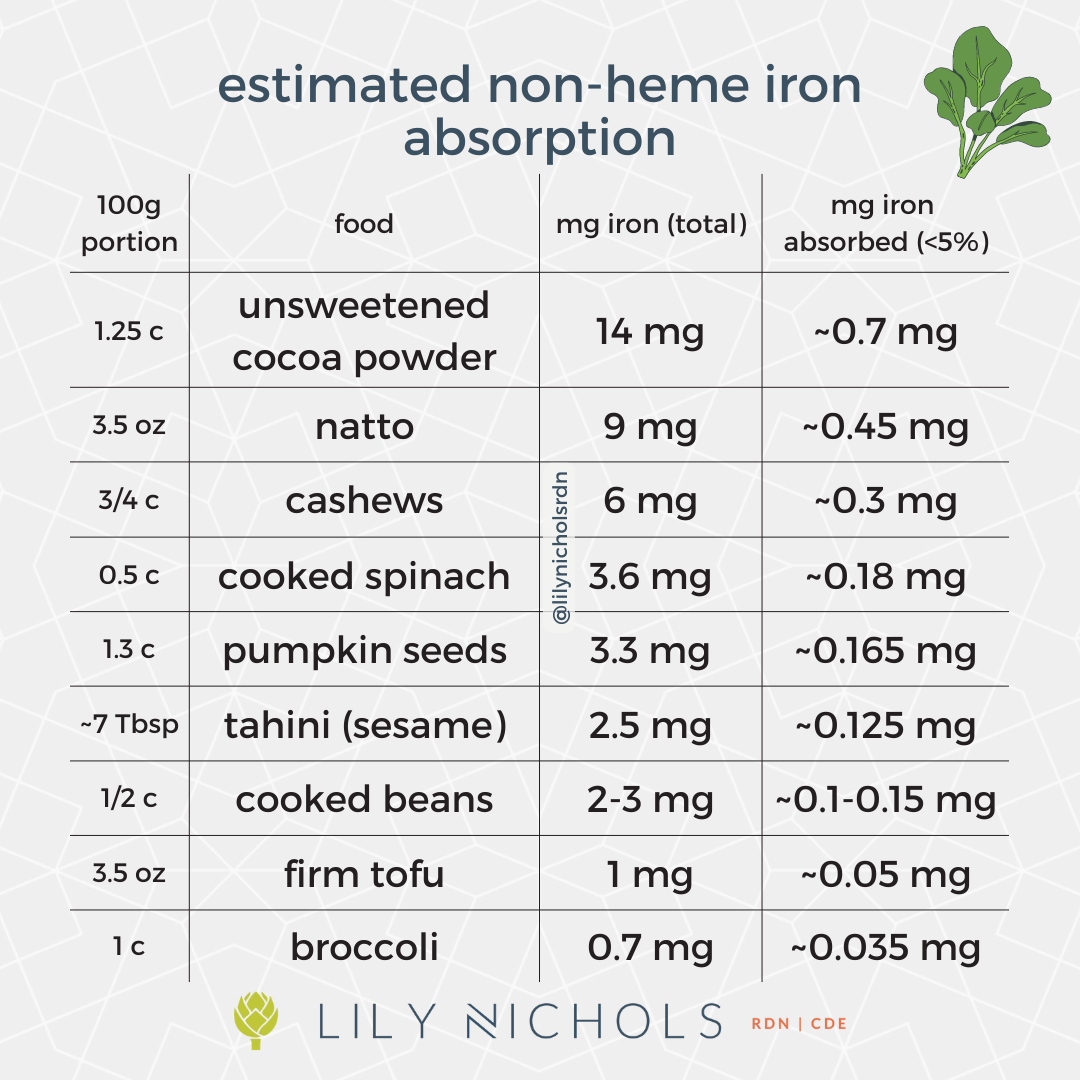
Non-heme iron is iron found mostly in plant foods like whole grains, leafy greens, nuts, seeds, and legumes (animal foods also contain small amounts of non-heme iron). The foods with the greatest concentration of non-heme iron per 100 g serving are: unsweetened cocoa powder, natto, cashews, cooked spinach, pumpkin seeds, tahini, cooked beans, firm tofu, and broccoli.
But before you start pounding the pumpkin seeds as your sole source of iron, you’ve gotta consider both the relative concentrations of iron per serving and the absorption from different foods. Make sure you check out the graphics in this article!
Relative Iron Absorption From Different Foods
As you may know, no vitamin or mineral is absorbed 100% when you consume it. That said, there are some forms of vitamins and minerals that are better absorbed.
Despite some non-heme iron foods having similar amounts of iron per portion as heme iron foods (i.e. cooked spinach to ground beef), the amount that’s absorbed can vary quite a bit.
Heme iron absorbs at a rate of about 25-40%. Non-heme iron absorbs at a rate of about 2-13% (average is <5%).
In the charts below, you’ll see the total iron content of foods in one column and the estimated iron absorption in the right column. Look closely!
What this means is that when you eat a serving of ground beef that contains 3.2 mg of iron, you’re only absorbing about 0.8 mg of iron (assuming 25% absorption). Whereas, if you eat half a cup of cooked spinach that contains 3.6 mg of iron, you’re only going to absorb 0.18 mg of iron (assuming 5% absorption). That’s >75% less iron absorbed than you’d get if you had ground beef.
You can visualize this in the example below. I estimated the absorption of heme iron to be 25% and the absorption of non-heme iron to be 5%.*
*This errs on the side of the lower range of heme iron absorption and to the average range for non-heme iron absorption (keep in mind that the non-heme iron absorption from grains is even lower, at only 0.3% to 1.8%).
I’ve included a number of head-to-head comparisons of animal and plant foods to show you that even if you match the iron content, you need a significantly larger portion of plant foods to match the amount of iron that is actually absorbed.
The challenge with non-heme iron absorption is that despite some plant foods often being high in iron, many of these foods contain other compounds that decrease the absorption of iron. Some examples are:
- Phytic acid (found primarily in beans/legumes, seeds, nuts, whole grains)
- Oxalates (found in foods like spinach, soy products, almonds, potatoes)
- Certain polyphenols, including tannins (found in vegetables, herbs, cereals, spices, tea, coffee, red wine, and cocoa)
- Fiber (found in beans/legumes, nuts, seeds, whole grains, and vegetables)
The differences in iron absorption from plant versus animal foods are precisely why there are higher rates of iron deficiency seen in vegetarians/vegans and also why there are separate, higher dietary iron recommendations for vegetarians/vegans. In fact, the RDA for iron is set 1.8x higher for vegetarians. Vegetarian women, on average, have lower iron stores and are more likely to be anemic.
Can You Boost Iron Absorption From Foods?
While inhibitors of iron absorption primarily affect non-heme iron, they can also impair the absorption of heme iron, just to a lesser degree. To offset this, research has identified a number of ways to enhance iron absorption from foods.
Polyphenols
Polyphenols are known to impair the absorption of iron. So even though foods with polyphenols have antioxidant properties that are generally good for you, if you’re trying to focus on absorbing as much iron as possible, you’ll want to strategize when you have polyphenol-rich foods and when you have iron-rich foods.
In one study, polyphenols inhibited iron absorption anywhere from 50% to 90%. That’s a lot! Now, not all polyphenols work the same and the amount of polyphenols consumed plays a role, too. But in general, it may be best to have iron at times you’re not having polyphenol-rich foods.
Since coffee and tea are some of the largest contributors to American’s polyphenol intake, this may look like not having coffee or tea at meals where you’re eating iron-rich foods OR when you take iron supplements. For example, if you take an iron supplement in the morning with coffee, it would be better to take it at a different time of day or with a different beverage.
Vitamin C
Although polyphenols make iron absorption more difficult, vitamin C can actually counteract some of the impact of polyphenols on iron absorption. For example, one study found that while polyphenols impair the absorption of iron (even for heme iron), regular consumption of vitamin C can counteract this effect, assuming that polyphenol intake is moderate.
Just how effective is vitamin C at enhancing iron absorption? Well, it depends on many factors (including the amount of vitamin C you consume and a person’s iron status), but one study found that consuming 100 mg of vitamin C (the amount of vitamin C in about 1.25 cups of broccoli) with a meal increased non-heme iron absorption by almost 3 times as much compared to iron consumed without vitamin C.
What this may look like for you is eating bell peppers, citrus fruits, kiwi, strawberries, and broccoli around the same time you consume iron-rich foods. Here are some specific food pairings ideas to help with iron absorption:
- Tomato sauce with ground beef (try the grass-fed beef meatloaf in Real Food for Pregnancy, which has lots of iron from not only the beef, but the hidden liver in it)
- Salsa served with beans
- Meat marinated in vinegar-based marinade
- Eating oranges or other citrus fruit with chicken or pork
- Having a broccoli side with steak or chicken
Calcium
Many minerals work synergistically, while others are antagonistic. Unfortunately, calcium impairs the absorption of iron, so it’s a best practice to have these two nutrients at different times.
One study found that consuming 165 mg of calcium (the amount of calcium in about half to one oz of cheese) with a meal reduced non-heme iron absorption by around 50% when calcium and iron were consumed together. Another study found that consuming 300 mg of calcium (the amount of calcium in about a glass of milk) with a meal reduced non-heme iron absorption by 49% and heme iron absorption by 39%.
It’s important to note that this same interaction occurs for calcium supplements or iron supplements. For example, if your clinician has recommended supplemental iron, don’t take your iron pill with a glass of milk. Likewise, don’t take a calcium supplement alongside an iron-rich meal.
Drawing from the previous point on vitamin C, if you instead take your iron supplement with a glass of water with lemon juice, you’d enhance iron absorption.
Cast Iron Pans
You can improve your iron intake not only from the type of foods you eat, but also how you cook them. Cast iron pans can sometimes “fortify” the foods you cook in them by leaching a little bit of the iron from the pan.
One study looked at the increase in iron content from foods cooked in cast iron pans. For cooked applesauce, the iron concentration increased by 16 times. For tomato sauce, it increased by 6.3 times. For scrambled eggs, it increased by 12.7 times. All of these were compared to their respective raw counterparts.
To get this effect, cooking time, temperature, and acidity of the food matter. More acidic foods will leach more iron from the pan. Even though you’ll just be adding a bit more iron to your foods with this cooking method, every bit counts when you’re treating iron deficiency!
Plus, cast iron is a much better option to cook in compared to toxic non-stick pans.
Nutrients That Support Iron Status
While these tips can definitely help maximize your iron absorption, having adequate nutrition overall is just as key to getting maximum iron intake. There are many micronutrients that are cofactors for iron metabolism. Without them, iron absorption and digestion can be suboptimal.
The amino acids found in meat have been shown to enhance iron absorption. Nutrients, like vitamin B12 and folate are directly involved in the creation of red blood cells. Therefore, intake of those two nutrients alongside iron has been shown to improve iron status and anemia better than iron alone. Similarly, vitamin A (as the retinol form, which is found in animal fats) as well as the mineral copper, are needed to support iron utilization, transport, and iron recycling within the body. Deficiencies in either of these can severely affect iron status. Luckily, when you’re focusing on increasing your heme iron intake, those very same foods often provide both of these nutrients, especially liver, organ meats, and shellfish. Zinc is also critical in the creation of heme (a part of hemoglobin). Again, animal foods are the best sources of bioavailable zinc.
If you’ve read my book, Real Food for Pregnancy, you likely already know the importance of eating well-balanced and nutrient-dense meals. Hopefully, this article has provided even more reason to prioritize your nutrition in pregnancy.
Summary
While there are a few tips and tricks to help optimize iron absorption from all foods, these strategies pale in comparison to eating foods that are rich in heme iron.
Animal foods are not only higher in iron by concentration, but are also much better absorbed than iron-rich plant foods.
You can certainly benefit from the iron in plant foods, but when it comes to correcting a deficiency or meeting the increased iron needs in pregnancy, nothing comes close to animal foods.
Remember, when it comes to optimizing iron intake:
- Ensure that you’re eating some sources of animal protein, especially the ones highest in iron (such as shellfish and organ meats)
- Pair citrus or other vitamin C-rich foods with iron-containing foods
- Try to have foods high in polyphenols and calcium at different times of the day than when you’re having iron-containing foods
- Focus on eating real foods as much as possible
What’s been your experience with iron in pregnancy? I’d love to hear about it in the comments.
Until next time,
Lily
References
- Erdman Jr, John W., et al. Present knowledge in nutrition. John Wiley & Sons, 2012.
- Breymann, C. “Iron deficiency anemia in pregnancy.” Seminars in Hematology 52(4) (2015): 339–347.
- Institute of Medicine. (2001). “Dietary Reference Intakes for vitamin A, vitamin K, arsenic, boron, chromium, copper, iodine, iron, manganese, molybdenum, nickel, silicon, vanadium, and zinc.” Washington, DC: National Academy Press.
- Hurrell, R., and I. Egli. “Iron bioavailability and dietary reference values.” Am J Clin Nutr 91(5) (2010): 1461S–1467S.
- Hurrell, R.F., et al. “Degradation of phytic acid in cereal porridges improves iron absorption by human subjects.” Am J Clin Nutr 77(5) (2003): 1213–1219.
- Hunt, J.R. “Bioavailability of iron, zinc, and other trace minerals from vegetarian diets.” Am J Clin Nutr 78(3) (2003): 633S–639S.
- Hurrell R.F., et al. “Inhibition of non-haem iron absorption in man by polyphenolic-containing beverages.” Am J Clin Nutr. 1989;49(3):546-551.
- Ma, Qianyi, et al. “Bioactive dietary polyphenols inhibit heme iron absorption in a dose‐dependent manner in human intestinal Caco‐2 cells.” Journal of food science 76.5 (2011): H143-H150.
- Hallberg, L et al. “The role of vitamin C in iron absorption.” International journal for vitamin and nutrition research. Supplement = Internationale Zeitschrift fur Vitamin- und Ernahrungsforschung. Supplement vol. 30 (1989): 103-8.
- Skikne BS, et al. “Calcium effects on iron absorption: clinical and experimental studies.” Am J Clin Nutr. (1989); 49(3):546-552.
- Quintaes, Kesia Diego, et al. “Mineral migration and influence of meal preparation in iron cookware on the iron nutritional status of vegetarian students.” Ecology of food and nutrition 46.2 (2007): 125-141.
- Siegel ER, et al. “Iron bioavailability from ferric pyrophosphate in cooked foods: a study using intrinsic and extrinsic labels in human subjects.” J Food Sci. 1991;56(1):53-58.
- Koury, Mark J., and Prem Ponka. “New insights into erythropoiesis: the roles of folate, vitamin B12, and iron.” Annu. Rev. Nutr. 24 (2004): 105-131.
- da Cunha, M., et al. “Effect of vitamin A supplementation on iron status in humans: A systematic review and meta-analysis.” Critical Reviews in Food Science and Nutrition 59(11) (2019): 1767–1781
- Collins, James F., et al. “Metabolic crossroads of iron and copper.” Nutrition reviews 68.3 (2010): 133-147.















Hi! I love Real Food for Pregnancy and your blog posts! I moved to Colorado last year (elevation of my city is around 6000 ft), and my doctor mentioned that pregnant women may be at higher risk for iron deficiency here. Would love to know if you’ve encountered this at all in your experience or research. Thanks in advance!
My labs come back “fine”, but we know those are suboptimal numbers and at 16 weeks pregnant, I’m very out of breath. I suspect I get too few micros in my diet! I appreciate these tips on iron!
The visual of the iron absorption of animal vs plant is so eye opening! Thank you so much for putting this together.
It really puts things into perspective about supposedly iron-rich foods!
Very eye opening, thank you for sharing! Looking at these absorption numbers, it seems like one would need to consume quite a bit of food daily to hit that 27mg mark.
Yes, it’s actually quite hard to meet and there is controversy as to whether the 27mg is really necessary during pregnancy given the enhanced absorption and how nearly impossible that level is to meet from diet alone. This is why you want to go by lab markers of iron status and iron metabolism to guide whether extra iron is truly needed.
I came across some of this info when introducing my baby to solids (not to have milk when he’s having meat), but I’ve forgotten about it – this is a great reminder! I always enjoy reading your posts, they’re well researched, clear and eye-opening – thank you!
I love the graphics! I was focusing on iron already during our fertility journey, together with other minerals, and my numbers were really good throughout pregnancy. I am not a fan of iron supplements and I often see that getting in all the minerals needed for its proper absorption help get the iron level up, especially copper, retinol and magnesium.
Thanks for the article, really useful. 🙂
Confused with the iron recommendations – is it 27mg of ‘content’ or 27mg of ‘absorption’ we should be aiming for? 27 mg absorbed seems like I’d need to eat a lot of liver/ bivalves to meet it each day!
27mg of iron CONTENT to aim for in a day. The RDA reflects dietary levels.
Thank you for clarification on that. I commented above and was trying to figure out today how on earth I was supposed to consume that much to meet absorbancy rates. I’m curious to know if makes a difference in how you consume things in absorbancy such as eating liver cooked, raw or taking dessicated beef liver capsules.
Excellent article, thank you for sharing your knowledge.
Despite eating iron rich foods I still developed anemia during pregnancy. To treat it I received an iron infusion because I didn’t tolerate oral iron supplementation.
I find this article particularly valuable for feeding my infant. Because he consumes relatively small amounts of solid food, serving iron rich foods, especially those with heme-iron, in certain combinations while avoiding others will maximize the amount of iron he absorbs. And because we eat the same foods, we will both benefit!
Yes, those foods are extremely valuable for meeting baby’s iron needs with the tiny portions they eat (along with many other micronutrients). See my article on Starting Solids for more info on first foods!
HI LILY!
Great article, like Every Time, what about vit C cooked in brocoli for ex, With Heat vit C are kill isn’t it? AND what about oxydation of iron supplément and polyphenol in Wine?
I wondered about heat destroying vitamin C as well. There are a few vitamins that are heat sensitive.
Thanks for this article! I like cooking in cast iron pans but a few of mine are so well seasoned that nothing sticks at all. I wonder if the seasoning level of the pan contributes to how much iron leaches into the food?
It does, as well as the acidity of the food and how long it sits in the pan. But I’d choose well-seasoned cast iron any day. Choosing foods rich in heme iron is a much more reliable contributor to iron intake than cast iron. It’s just one extra way to boost intake a bit more.
Hi Lily,
Thank you so much for this helpful article! Im 28 weeks & my Iron came back low this week even though I feel like Im eating nonstop proteins. I also have RLS which has been unbearable.
I am taking FullWell thanks to your recommendation and the Iron Supplement my midwife recommended has extra folate, Vit C, and 30mg of B12 (which would be in addition to the 150mg in Fullwell). I just dont want to overdo it. Do you have any recommendations for an Iron Supplement that I can just drink with a glass of water with some lemon?
Thank you SO much.
Seeking Health has some options for iron (search iron on their site): https://www.seekinghealth.com/?rfsn=2719643.0e875c&utm_source=refersion&utm_medium=affiliate&utm_campaign=2719643.0e875c
You can also check my Fullscript for some other iron supplement options that you can discuss with your provider.
Also, keep in mind that some other nutrients can influence risk of RLS, which I covered in this research brief.
You are the best. Thank you so much as always!
p.s. I think I may have failed my 3 hr Glucose test this pregnancy as well this past week but instead of feeling lost and scared, I feel so empowered with all the knowledge you gave me during my last pregnancy with your book. I shared your book with all the women waiting next to me in the waiting room during the 3hr test. 🙂
xoxo
So glad it gave you some peace of mind. It’s a diagnosis nobody wants, but it’s manageable and sometimes there’s a silver lining in the end.
Thank you for this very helpful article, Lily! Do you have recommendations for what optimal iron and ferritin labs look like before and during pregnancy?
Thanks!
Annie
Perfection as usual Lily. Loved the iron content vs. absorption charts.
Love the article and also love my piece of dark chocolate and green tea after a meal (eat meat for lunch en dinner). How long do you have to wait with consuming tea and choclate to not mess up your iron intake of that meal?
I haven’t seen studies looking specifically at this. My guess is probably about an hour post meals or 30 min before.
I heard you on the midwives cauldron podcast during my first pregnancy in 2022 and then bought real food for pregnancy (unfortunately on Audible…I am thinking of getting the hard copy now!) …. I hand-wrote out a lot of the recipes but I can’t find them now! I did know the pate recipe by heart at one point haha.
Fast forward to second pregnancy and I am low in iron for the first time in my life! You are such a blessing. I was feeling so overwhelmed – wanting to follow the midwives advice and start on iron supplements ASAP but also thinking I need to make some dietary changes and this article REALLY helped. I had a PPH my first birth so wanting to get on top of my stores this time around. Appreciate your work so very much.
Hi Lily, we are due with our first baby, and I was talking to my husband about wanting to avoid supplements, and instead get it nutrients I need through foods. The next day I came across your book! Thank you for putting in the time and research so we can have as natural a pregnancy as possible!
I do have a question, you make the example of not drinking coffee with breakfast high in iron. How far apart should my intake of Polyphenols or calcium be from iron?